Clinical Application of Hyperbaric Oxygen Therapy for Diabetes and Its Complications
Hubei Journal of Preventive Medicine, Volume 12, Issue 6, 2001
Objective
The 20 cases in the hyperbaric oxygen therapy group for diabetes and the 20 cases in the control group for diabetes were all inpatients and outpatients of Dongfeng Motor Company General Hospital, in accordance with the 1980 World Health Organization (WHO) diagnostic criteria for diabetes. In the hyperbaric oxygen therapy group, there were 12 males and 8 females, aged 38 to 69, with an average age of 53.5 years, and a disease duration of 2 months to 10 years, with an average of 5 years. Among them, 3 had concomitant hypertension, 2 had cerebral infarction, 2 had coronary heart disease, and 1 had skin disease. In the control group, there were 13 males and 7 females, aged 35 to 71, with an average age of 53 years, and a disease duration of 1 month to 9 years, with an average of 4.5 years. Among them, 2 had concomitant hypertension, 2 had coronary heart disease, 3 had cerebral infarction, and 1 had peripheral neuritis. All 40 cases were type II diabetes patients.
Methods
All 40 patients received controlled diet, symptomatic treatment, anti-infection treatment, and antihypertensive treatment. In the hyperbaric oxygen therapy group and the control group, 4 and 3 cases received insulin injections, respectively, and the others took oral hypoglycemic agents such as metformin and gliclazide for treatment. The hyperbaric oxygen therapy group used large hyperbaric oxygen chambers, with a pressure increase of 20 minutes, a stable pressure maintenance with pure oxygen inhalation for 60 minutes, a 10-minute rest period, and a pressure decrease of 20 minutes, with a pressure of 0.2 MPa, once a day. Ten treatments were considered as one course of treatment, and 1 to 2 courses of treatment were given based on the condition. Before and after treatment, fasting for 12 hours, venous blood was taken to measure fasting plasma glucose, total cholesterol, triglyceride, low-density lipoprotein, and 24-hour urine protein quantitation.
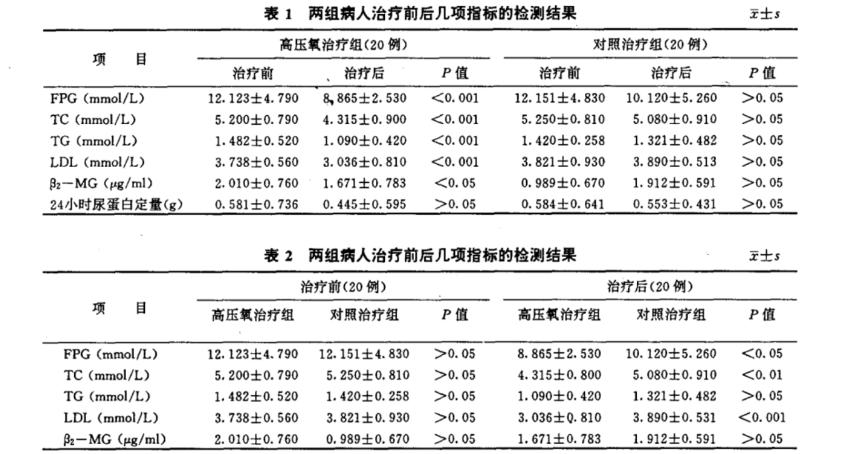
After hyperbaric oxygen combined treatment, the levels of FPG, TC, TG, and LDLB-MG were significantly reduced compared to before treatment, with highly significant differences observed through statistical analysis (P<0.001 P<0.05). In the control group, although there was a decrease in each value after treatment, there was no significant difference when comparing before and after treatment (P>0.05) (Table 1).
After treatment, there was a significant difference in fasting plasma glucose, total cholesterol, and low-density lipoprotein between the hyperbaric oxygen group and the control group, indicating that hyperbaric oxygen therapy has a certain effect on the disorder of lipid metabolism in diabetes (Table 2).
The occurrence of lipid metabolism disorder syndrome in diabetes is one of the important causes of various diseases. When blood glucose is properly controlled, the levels of blood lipids will decrease as the condition improves, and the decrease in fasting plasma glucose is positively correlated with the decrease in total cholesterol, triglyceride, and low-density lipoprotein. In this group, the decrease in total cholesterol, triglyceride, and low-density lipoprotein after hyperbaric oxygen therapy is related to the decrease in blood glucose level, and the decrease is more significant compared to the control treatment group, which is related to the acceleration of lipid breakdown by hyperbaric oxygen.
According to the research by Kakhnovskii et al., hyperbaric oxygen therapy inhibits the action of insulin-inhibiting hormones (growth hormone and glucagon), corrects acid-base imbalance, increases the secretion of S-peptides, improves tissue sensitivity to insulin, and increases tissue oxygen supply due to the doubling of blood oxygen concentration and the diffusion distance of oxygen in tissues. As a result, the oxygen content in the patients' bodies increases, tissue cell vitality enhances, aerobic metabolism becomes vigorous, leading to increased glucose consumption and a decrease in blood glucose.
The glomerular filtration rate, proximal tubular reabsorption function, and urinary protein excretion of diabetic patients have significant differences compared to normal individuals, especially when combined with diabetic nephropathy, the B-MG content in the blood of patients increases. It is generally believed that tissue hypoxia in diabetic patients can exacerbate the development of microvascular lesions, leading to further worsening of microcirculation disorders. Hyperbaric oxygen can improve the symptoms of renal ischemia, increase glomerular filtration rate, correct tissue hypoxia, and improve microcirculation disorders, etc. Therefore, the decrease in B-MG after hyperbaric oxygen therapy is more significant compared to the control group.
According to the clinical observations of this treatment, the insulin dosage of 4 patients in the hyperbaric oxygen therapy group decreased by 4-20 units and their condition stabilized. Before treatment, these patients experienced blood sugar fluctuations that were difficult to control with routine medications. After 10 sessions of hyperbaric oxygen therapy, blood sugar gradually decreased and stabilized, and clinical symptoms improved. The improvement of symptoms is related to the increase in oxygen partial pressure and physical dissolved oxygen levels caused by hyperbaric oxygen therapy, as well as the correction of tissue hypoxia, which promotes the generation of collateral circulation.
In conclusion, hyperbaric oxygen therapy has practical significance in the treatment of diabetes and the prevention of complications.
References:
1. Zhu JM. The diagnostic value of serum and urinary 2-microglobulin determination for diabetic kidney disease. Journal of Xi'an Medical University, 1986, 7(11).
2. Chen MZ. Chinese Internal Medicine (Volume II). Beijing: People's Publishing House, 1999.
3. Yang LH. Clinical application of hyperbaric oxygen therapy for diabetes. Hyperbaric Oxygen Medicine Journal, 1996, 5(2): 108-109.
4. Li CQ. Comprehensive treatment of diabetes with hyperbaric oxygen. Chinese Journal of Endocrinology and Metabolism, 1992, (3): 175.
The effectiveness of hyperbaric oxygen chambers in treating diabetic foot patients has been confirmed by the official website of the United States:
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2858192/
The Food and Drug Administration (FDA) has given HBOT approval for the treatment of 13 conditions, including wounds such as diabetic foot ulcers. The Undersea & Hyperbaric Medical Society also lists HBOT as a treatment option for diabetic foot ulcers.
Clinical trials in the United States (including data comparison):
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2858204/

Discount Price, ship by DHL, door to door service, 5-7days delivery time, local technical support

We supply soft and hard chambers from 1.3-2.0ATA to reach different customers' needs

Create custom uniquea hyperbaric chambers to reach your target market

We have more than 50 distributors around world, looking forward to having you on board.