Why Hyperbaric Oxygen Chamber Can Treat Trauma?
Hyperbaric oxygen therapy is effective in treating wounds because it promotes wound healing by addressing key factors involved in the process. Healing any wound requires adequate blood flow and oxygen supply, and the rupture of blood vessels can lead to local hypoxia, a crucial factor limiting wound healing. Hyperbaric oxygen therapy increases blood oxygen tension and oxygen content, improving the oxygen-deficient state of damaged tissues. It also constricts blood vessels, promotes the establishment of collateral circulation, enhances the bactericidal action of white blood cells, and improves their ability to engulf pathogens and remove necrotic tissue, all of which facilitate wound healing.
Hyperbaric oxygen therapy increases blood oxygen partial pressure, oxygen content, and the effective diffusion distance of oxygen. This rapidly corrects the hypoxic condition at the wound site and promotes the formation of new blood vessels and granulation tissue growth, as well as modulating the body's immune response, all of which contribute to wound healing.
It reduces pathological inflammatory responses, alleviates tissue swelling, and controls wound infections.
It promotes blood vessel constriction through an adrenaline-like effect, reducing local blood volume and aiding in the reduction of tissue edema following trauma.
When we think of wounds, we often imagine cuts and lacerations that bleed, which can be quite unsettling. However, aside from bleeding wounds, there are various other types of injuries we may encounter. For example, we might accidentally bump into something and develop a bruise without any broken skin or bleeding. Alternatively, in cosmetic procedures, minor "injuries" to the deep layers of the skin are intentionally induced to stimulate regeneration, benefiting the renewal of skin cells.
Certainly, we can refer to these "injuries" as internal injuries because they don't involve damage or bleeding on the skin's surface. These internal injuries may involve some level of damage to the skin's deeper layers, muscle tissue, and capillary network, and in some cases, the damage may result in visible bruising on the skin's surface. In everyday life, we often experience situations where we develop a "black and blue" mark after bumping into something, which is caused by the rupture of capillaries within the muscle tissue, leading to bleeding.
For these types of injuries, there is typically no need for bandaging, as they will gradually heal on their own. The speed of recovery depends on factors such as local microcirculation, nutritional status, age, and daily care. To achieve better recovery, taking measures early on tends to yield more effective results, much like applying an ice pack immediately after undergoing a procedure like a picosecond laser treatment.
The process of wound healing is complex and closely related to inflammation, blood vessel formation, collagen production, re-epithelialization, and wound closure after shaping. Systemic factors such as age, nutritional status, coexisting medical conditions, the severity of the injury, and the local environment of the wound (bacterial infections, wound moisture level, local oxygen tension, and blood supply) all have a significant impact on wound healing. Oxygen supply to the wound is one of the key factors, and hypoxia is a common cause of impaired wound healing.
Hyperbaric oxygen therapy, as an effective method to correct hypoxia, has been used since as early as 1965 to promote wound healing. In recent years, it has gained increasing attention and recognition for its application in various types of injuries, including chronic wounds, diabetic foot ulcers, endangered skin flaps and grafts, crush injuries and compartment syndrome, radiation-induced soft tissue injuries, burns, traumatic brain injuries, and more.
Hyperbaric oxygen therapy contributes to wound healing through several processes: it increases blood oxygen partial pressure, oxygen content, and the effective diffusion distance of oxygen, rapidly correcting the hypoxic state at the wound site and reducing ischemia-reperfusion injury. It also reduces pathological inflammatory responses, alleviates tissue swelling, and controls wound infections. Additionally, it promotes the formation of new blood vessels and granulation tissue growth, as well as modulating the body's immune response, all of which contribute to wound healing. While most wounds can achieve satisfactory healing results through conventional treatments such as debridement, dressing changes, vascular reconstruction, antibiotic application, nursing care, and nutritional support, in the case of hypoxic wounds, hyperbaric oxygen therapy, when combined with infection control, effective debridement, appropriate dressing changes, and correction of vascular disorders, can significantly enhance the healing process.

In February 2020, an interesting article was published in "Nature's" Scientific Reports:
Scientists conducted research on the early recovery of muscle injuries (bruises) promoted by Hyperbaric Oxygen (HBO) therapy. One key mechanism of HBO is the upregulation of Reactive Oxygen Species (ROS). ROS can increase oxygen solubility at high pressure, leading to high oxygen content in tissues. Nitric oxide (NO) is one type of ROS that can stabilize Hypoxia-Inducible Factor (HIF) 1α, stimulating the secretion of vascular endothelial growth factor (VEGF) and basic fibroblast growth factor (bFGF) by endothelial cells and macrophages, thereby inducing blood vessel formation.
The study aimed to investigate whether HBO could promote vascular regeneration in rats' skeletal muscles following contusions and induce muscle regeneration. The HBO treatment regimen included 2.5 atmospheres of pressure with 100% pure oxygen for 120 minutes, once daily, for five consecutive days. HBO significantly increased levels of NO, VEGF, and bFGF, stabilizing HIF1α within one day. HBO promoted blood vessel formation from days 3 to 7 after the contusion and muscle healing from days 5 to 7. Therefore, in the early stages of muscle contusions (internal injuries), HBO primarily promotes vascular regeneration and muscle regeneration through NO generation.
From this study's results, two clear conclusions can be drawn: first, tissue oxygen concentration increases under high pressure, and second, HBO promotes blood vessel formation and muscle healing at the site of injury. This is why, in clinical practice, patients with difficult-to-heal wounds (such as diabetic foot ulcers) are placed in hyperbaric oxygen chambers to promote wound healing.
This is good news for individuals interested in aesthetics. With the widespread popularity of medical aesthetic procedures, post-procedure recovery has become a crucial factor in the success of these procedures.
A decade ago, when we talked about medical aesthetics, we often thought of "big procedures" like rhinoplasty, facial bone contouring, and breast augmentation. Nowadays, medical aesthetics have evolved significantly, with a wide range of innovative procedures available. In addition to major procedures, there are also many refined and effective "minor procedures" such as Thermage, ultrasound knife, and peeling. Regardless of whether it's a major or minor procedure, some muscles or blood vessels are damaged, and after repairing these damaged vessels and muscles, a micro-reconstruction effect is achieved, revealing a new appearance. With the assistance of hyperbaric oxygen, the repair of blood vessels and muscles can be faster and more complete, accelerating the achievement of the most perfect aesthetic results.
Therefore, hyperbaric oxygen therapy, besides treating conditions like carbon monoxide poisoning and stroke, can also be applied in skincare and post-medical aesthetic procedures, making it a boon for individuals interested in aesthetics.
[Case Study]
In April 2022, Mr. Feng underwent internal fixation surgery for a left foot fracture due to poor blood circulation and a lack of fat and muscle tissue around the bone area. The wound was difficult to heal, and post-surgery, his left foot appeared red and swollen, and the wound turned black. The doctor recommended that he try hyperbaric oxygen therapy.
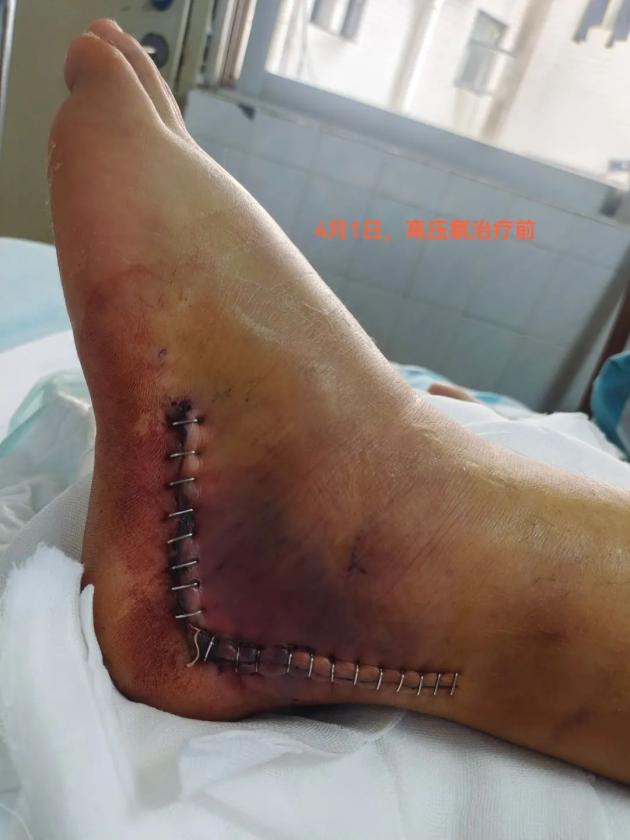
"I've only heard of hyperbaric oxygen therapy for treating carbon monoxide poisoning. Can it also help with wound recovery?" Mr. Feng was filled with doubts, but he decided to follow the doctor's advice and underwent hyperbaric oxygen therapy at the Huizhou Central People's Hospital. To his surprise, after just two sessions of hyperbaric oxygen therapy, the swelling in his left foot had subsided, and his wound had noticeably healed!
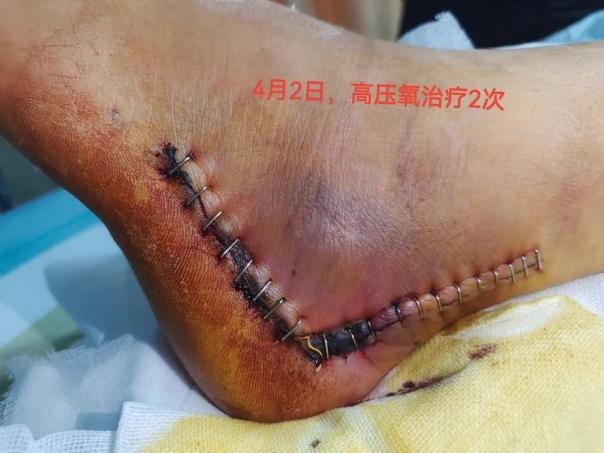
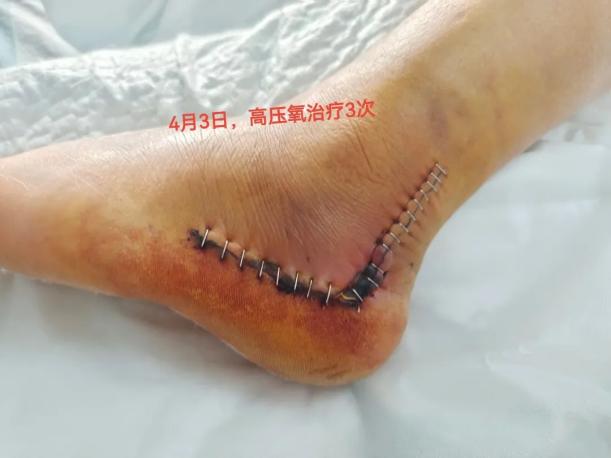
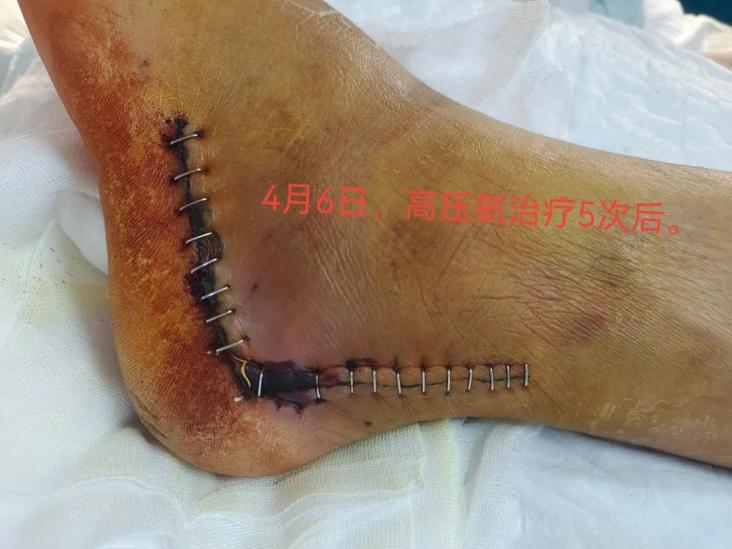
Mr. Feng, in his joy, didn't forget to ask the doctor why hyperbaric oxygen therapy can help with wound healing. Dr. Zhu Ruifang, Director of the Hyperbaric Oxygen Department at the Central People's Hospital in the city center, provided a detailed explanation.
Hyperbaric oxygen therapy (HBOT soft chamber) involves breathing pure oxygen or high-concentration oxygen under an environment with pressure higher than one atmosphere to treat various medical conditions. As an effective physical therapy for correcting hypoxia, HBOT has been used since as early as 1965 to promote wound healing and has been successfully applied in the treatment of both acute and chronic wounds. Its mechanism of action includes improving neovascularization, reducing the production of pro-inflammatory cytokines, and increasing the synthesis of growth factors and collagen. Specifically, the mechanisms by which hyperbaric oxygen promotes wound healing include the following aspects:
Increasing tissue oxygen tension: In cases of trauma, tissue cells swell, and the distance between cells and capillaries increases, leading to reduced oxygen supply. Breathing oxygen at normal pressure cannot raise the oxygen tension or improve the diffusion distance of oxygen. Under hyperbaric oxygen conditions, due to the increased pressure, a significant amount of oxygen dissolves in the blood, increasing the oxygen carried into ischemic tissues, effectively addressing the hypoxic condition mentioned earlier.Furthermore, wound healing relies heavily on the proliferation of fibroblasts and the production of substances such as collagen. Severe ischemia and hypoxia can lead to slow or halted fibroblast growth. Hyperbaric oxygen increases oxygen supply to the wound, promoting fibroblast proliferation and the accumulation of collagen.
Promoting blood vessel constriction: Hyperbaric oxygen has an alpha-adrenergic-like effect that causes blood vessels to constrict. This reduces the local blood volume, which is beneficial for reducing tissue swelling after trauma.
Inhibiting anaerobic bacteria and enhancing leukocyte function: Inhaling oxygen at high pressure (3 atmospheres) can raise tissue oxygen tension at the lesion site to 300 mmHg (42.9 kPa), effectively inhibiting the growth and activity of anaerobic and aerobic bacteria. Research has shown that hyperbaric oxygen treatment at 2.5 atmospheres can significantly inhibit the growth of tuberculosis bacteria.
Hyperbaric oxygen therapy also enhances the bactericidal action of white blood cells (leukocytes). After engulfing bacteria, white blood cells consume oxygen at a significantly increased rate. Hyperbaric oxygen therapy, by increasing oxygen supply to white blood cells, markedly enhances their phagocytic activity.
In summary, wound healing requires sufficient blood perfusion and oxygen supply, and a home hyperbaric oxygen chamber provide higher oxygen levels than usual. Moreover, at pressures above one atmosphere, oxygen is absorbed more effectively by the patient. Therefore, hyperbaric oxygen chambers can contribute to better and faster wound healing. Animal experiments have shown that hyperbaric oxygen promotes blood vessel formation from days 3 to 7 after contusions and muscle healing from days 5 to 7. Thus, in the early stages of muscle contusions (internal injuries), hyperbaric oxygen primarily promotes vascular regeneration and muscle regeneration. In real-life cases, it also offers advantages like increasing tissue oxygen tension, promoting blood vessel constriction, and enhancing leukocyte function.

Discount Price, ship by DHL, door to door service, 5-7days delivery time, local technical support

We supply soft and hard chambers from 1.3-2.0ATA to reach different customers' needs

Create custom uniquea hyperbaric chambers to reach your target market

We have more than 50 distributors around world, looking forward to having you on board.