In recent years, the incidence of traumatic brain injury (TBI) caused by motor vehicle accidents, falls, violence and blunt trauma has increased. Impairment of brain function caused by trauma may be permanent, leading to emotional, cognitive, and movement disorders. The primary brain injury is irreversible. Most novel and effective treatment strategies focus on the secondary brain injury process caused by immune activation. A series of cellular and molecular changes play an important role in these cascades, leading to excitotoxicity neuroinflammation, and ultimately leading to apoptotic cell death of neurons and glia.
Extracellular histones have been identified as a key factor in the subsequent inflammatory process of tissue damage caused by hypoxia and ischemia. Hyperbaric oxygen therapy (HBOT) patients inhale pure oxygen or high-concentration oxygen in an environment maintained at more than one atmosphere, which is widely used in clinical practice for TBI. A large number of studies have shown that HBOT can reduce secondary brain damage in brain injury by improving oxidative metabolism and reducing neuroinflammatory response. The neuroprotective effects of HBOT may be manifested in preserving mitochondrial integrity, inhibiting mPTP and reducing mitochondrial apoptosis.
Hyperbaric oxygen therapy: The hyperbaric chamber is perfused with pure oxygen for 5 minutes, and then the pressure is increased to 1.6 and 2.2 atmospheres respectively within 10 minutes. The patient inhales hyperbaric oxygen for 60 minutes at a steady pressure and then decompressed for 15 minutes. During HBO treatment, the hyperbaric chamber is continuously ventilated at a rate of 8-10L/min to prevent CO2 accumulation and maintain the oxygen concentration at 95%. The temperature of the lying type hyperbaric chamber is maintained at 22 to 26°C, and the humidity is maintained between 40 and 50%.
Figure 1 Using the mNSS score test to evaluate the neurological changes of TBI
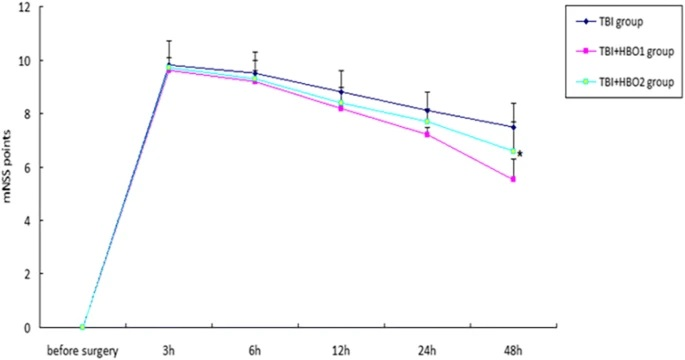
TBIgroup traumatic brain injury group; TBI+HBO1 traumatic brain injury+1.6ATA hyperbaric oxygen treatment group; TBI+HBO2 traumatic brain injury+2.2ATA hyperbaric oxygen treatment group
As shown in the figure, 1.6ATAHBOT significantly improved the early neurological recovery of TBI.
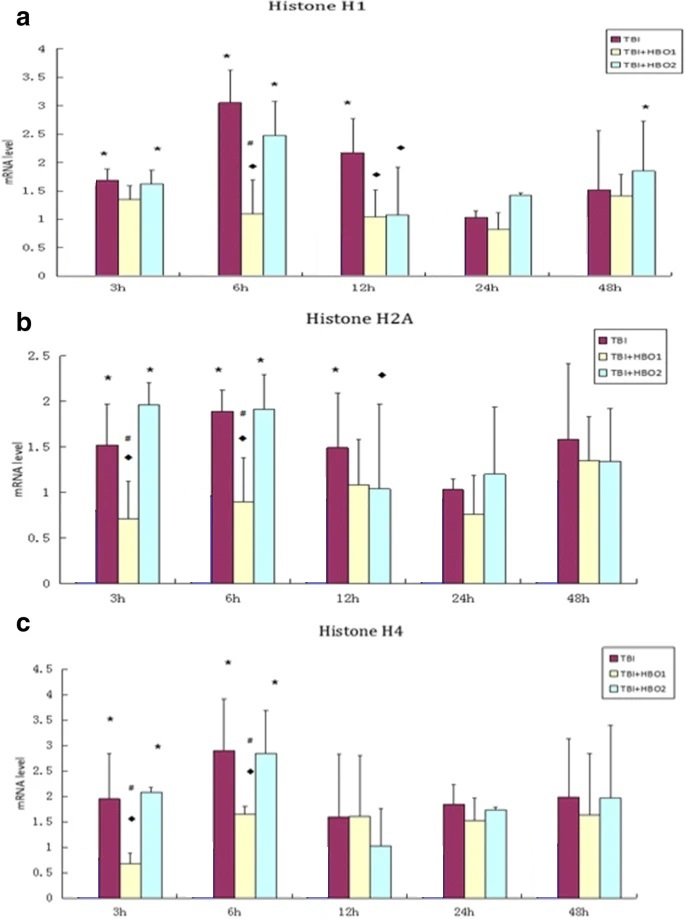
HBOT stroke recovery attenuated the mRNA and protein expression of extracellular histones H1, H2A and H4 after TBI. The histone decline of the 1.6ATA group was significantly lower than that of the 2.2ATA group, especially in the early stage. In general, compared with 2.2ATA, 1.6ATAHBOT intervention can more effectively inhibit the release of extracellular histones in brain tissue induced by TBI in the early stage of injury.
Apoptotic cell death of neurons is a sign of secondary brain injury. In order to evaluate the effects of different ATAHBOTs on cell apoptosis induced by extracellular histones, we analyzed the apoptosis index of each group.
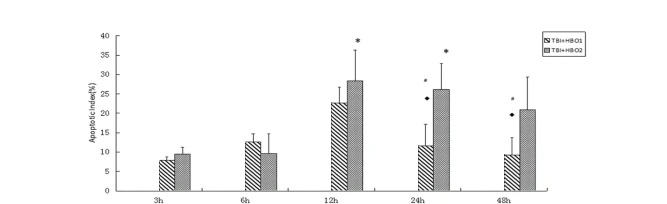
HBOT has been proven to promote neuron survival and regulate neuroinflammation by reducing oxidative stress, thereby reducing cell apoptosis in brain injury. It is preliminarily confirmed that 1.6ATAHBOT may inhibit histone release more effectively than 2.2ATAHBOT, thereby reducing the secondary brain injury of TBI.
The results of the study show that early treatment with relatively low pressure (1.6ATA) hyperbaric oxygen can significantly inhibit the expression of extracellular histones H1, H2A, H4 and NF-κB around the lesion, reduce nerve cell apoptosis, and thereby play an important role in reducing secondary brain injury.
https://link.springer.com/article/10.1007/s12192-020-01137-6
Macy-pan has quality hyperbaric oxygen therapy for sale, you can send a email to rachel@macy-pan.com or dial at 0086-180-1702-3916 if interested.

Discount Price, ship by DHL, door to door service, 5-7days delivery time, local technical support

We supply soft and hard chambers from 1.3-2.0ATA to reach different customers' needs

Create custom uniquea hyperbaric chambers to reach your target market

We have more than 50 distributors around world, looking forward to having you on board.